10 Things to observe for PUI and PUM COVID-19 quarantine hospitals
As the national government explored and evaluated the viability of wide and open spaces such as the Philippine International Convention Center (PICC), Rizal Memorial Coliseum, World Trade Center, and Clark, the public raised questions about cross-contamination, proper distancing, and ventilation among others. Dan Lichauco of Archion Architects—who specializes in healthcare architecture and is currently working with the Department of Public Works and Highways, the Razon Group, and the Bases Conversion and Development Authority on the conversion of the PICC, Rizal Memorial Coliseum, and Clark—answered such queries on his Facebook post.
Here are 10 factors to consider when converting structures into COVID-19 quarantine hospitals based on Lichauco’s recommendations:
1| Isolation
Lichauco stressed that the objective of COVID-19 quarantine hospitals is to allow for the isolation of possible and confirmed COVID-19 cases to prevent contamination of healthcare workers and other patients. “This will require a (scaled down) medical team that may be augmented by volunteers. The medical team should be able to identify and anticipate potential severe cases and ship them out before they get worse. As a gauge, any patient who needs more than tanked oxygen should not be there,” explained the architect.
2| Transmission
The novel coronavirus spreads primarily through respiratory droplets and contact routes, and possibly through short-range aerosol transmission. According to the World Health Organization, “airborne transmission may be possible in specific circumstances and settings in which procedures or support treatments that generate aerosols are performed.” Hence, Lichauco advises that authorities must choose structures without carpets and air-conditioning. However, if there is no other choice, the architect suggests to “cover the carpet with linoleum or other roll vinyl products.” If the structure is air-conditioned, he suggests “open the window to get rid of some air and make sure there are at least six (6) air changes an hour, and do not re-circulate contaminated air or”
3| Ventilation
“Structures with good natural ventilation are preferred,” says Lichauco. He explains further, “Air can be moved, via electric fans, in a unidirectional manner from one end of the room to another. The virus will die in sunlight.” (You might like: LOOK: DIY COVID-19 home isolation room explained by a healthcare architect)
4| Sanitation and waste management
A WHO technical brief on water, sanitation, hygiene, and waste management for the COVID-19 virus states: “The risk of catching the COVID-19 virus from the faeces of an infected person appears to be low. There is some evidence that the COVID-19 virus may lead to intestinal infection and be present in faeces . . .However, to date only one study has cultured the COVID-19 virus from a single stool specimen (7). There have been no reports of faecal−oral transmission of the COVID-19 virus.” While there is risk, however low, Lichauco recommends traditional toilets and assures that there is no need for medical waste treatment facilities.

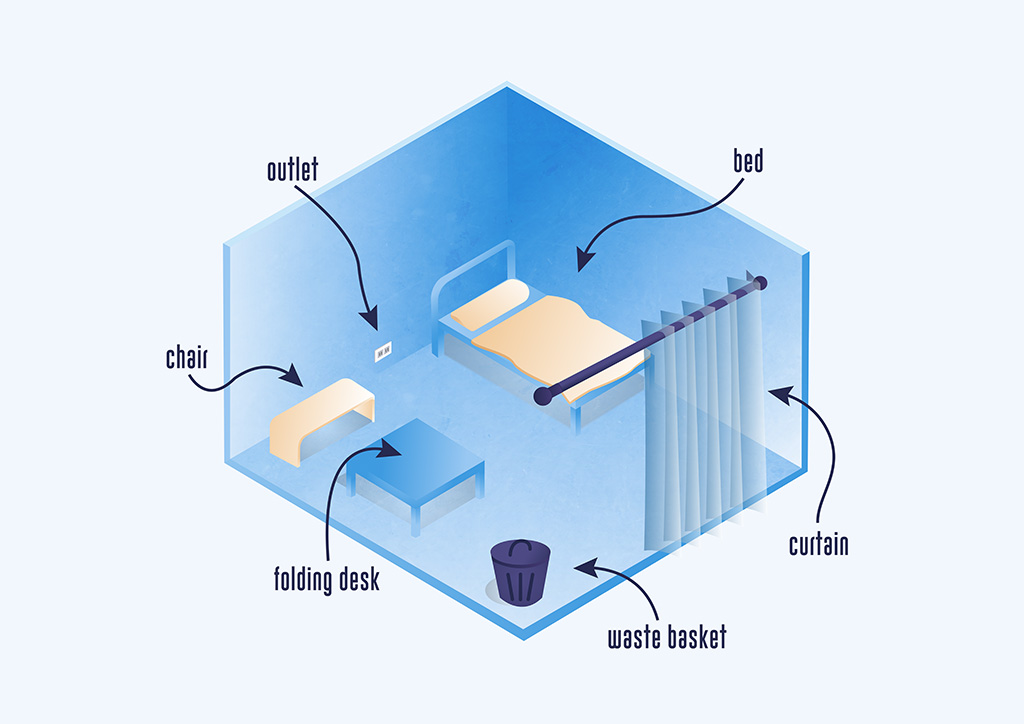
5| Bed distancing
Transmission occurs within 1-2 meters, which means a “bed should be 2.5 meters on center or further. Panel segregation is preferred for privacy and prevention of the droplets from going to the next cubicle” says Lichauco. The DOH epidemiologist’s recommended bed arrangement in COVID-19 quarantine hospitals is as follows:
- Bed size – 0.90 meters x 2.00 meters
- Bed spacing – 1.80 meters
- Space per patient – 2.70 meters x 3.80 meters
- Ideal area per patient – 10.26 square meters
6| Back of house entrance
The architect suggests use of structures with separate back of house entrances for delivery and assembly of food and supplies. “A separate garbage path will be preferred. Facilities with attached kitchens are even better. Hence, schools are ideal,” Lichauco furthers.

7| Location
Learning from the rejection of Marikina’s proposed COVID-19 testing center by the Department of Health (DOH), structures used for any COVID-19 matter should not be a mixed-use building, attached to non-COVID-19 facilities, and located in a densely populated area to avoid contamination. As much as possible, the structures should be located beside or near a hospital. Lichauco says quarantine tents by the hospital are good options as well. (You might like: An architect and a landscape architect suggest use of Quezon Institute as COVID-19 hospital)
8| Visitors
Persons in quarantine are not allowed to have visitors. However, Lichauco says (in a separate post) that a visitor center may be set up to exchange clothes and supplies.
9| Referral
The converted COVID-19 quarantine hospitals should have a partner hospital where severe cases may be referred to, according to Lichauco. Twelve (12) hospitals are mandated by the DOH to treat COVID-19 patients, while the Lung Center of the Philippines, Rodriguez Hospital, and the University of the Philippines-Philippine General Hospital are identified as the main hospital referrals for moderate to critical cases.
10| De-load overcapacity hospitals
Finally, Lichauco says, “The quarantine hospital is now one of the best ways to prevent the spread of the virus and de-load the hospitals. Step down hospitals should also be considered. Since the average stay is 12 days, after the 9-10th day the patient is well and waiting for their test result. A step down facility where the patient can be moved to will free up the coveted hospital beds. Filipino architects and private individuals have designed emergency quarantine facilities and raised funds to build them. WTA Architecture and Design, John Ryan Santos + Partners, PDP Architects, and Lichauco’s firm Archion Architects are among those who have shared their proposals.![]()